
More than 46 million, nearly 21% of adults in the United States, smoke, according to a 2010 report by the U.S. Centers for Disease Control and Prevention (CDC). Smoking kills more than 5 million people a year worldwide, accounting for 1 out of every 10 adult deaths.
Health Effects of Smoking
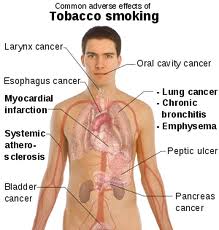
- Up to 90% of lung cancer deaths are attributed to smoking.
- Smoking greatly increases a person’s risk of heart attacks and strokes.
- COPD is directly related to smoking.
- Smoking greatly increases the smoker’s risk of oral and esophageal cancers.
- Women who smoke tend to start menopause at an earlier age than nonsmokers, perhaps because toxins in cigarette smoke damage eggs.
- Women who smoke have a greater risk for ectopic pregnancy and miscarriage.
- Smoking clearly increases the risk of colorectal cancer and aggressive colon polyps, which are considered precursors to colon cancer.
Nicotine Addiction

Nicotine is the chemical in cigarettes that makes them addictive. About 85% of smokers are addicted to nicotine. Higher levels of nicotine in a cigarette can make it harder to quit smoking. The amount of nicotine in cigarettes has steadily increased in the past decade. Higher nicotine levels have been found in all cigarette categories, including “light” brands. Some researchers feel nicotine is as addictive as heroin. In fact, nicotine has actions similar to heroin and cocaine, and the chemical affects the same area of the brain. Depending on the amount taken in, nicotine can act as either a stimulant or a sedative. Cigarette smoking has definite immediate positive effects. For example, it can:
- Boost mood and relieve minor depression.
- Suppress anger.
- Enhance concentration and short-term memory.
- Produce a modest sense of well-being.
Most smokers have a special fondness for the first cigarette of the day because of the way brain cells respond to the day’s first nicotine rush. Nicotine, particularly taken in the first few cigarettes of the day, increases the activity of dopamine, a chemical in the brain that elicits pleasurable sensations. This feeling is similar to getting a reward. Over the course of a day, however, the nerve cells become desensitized to nicotine. Smoking becomes less pleasurable, and smokers may be likely to increase their intake to get their “reward.” A smoker develops tolerance to these effects very quickly and requires increasingly higher levels of nicotine. Nicotine dependance refers to the development of symptoms with the sudden interruption or pronounced reduction in nicotine consumption for 24 hours or more.
Smokeless Tobacco

Smokeless tobacco, also called spit tobacco, includes chewing tobacco (dip and chew), tobacco powder (snuff), as well as flavored tobacco lozenges. These products also contain nicotine. Smokeless tobacco products allow tobacco to be absorbed by the digestive system or through mucus membranes. Smokeless tobacco contains at least 28 cancer-causing substances, and is not a safe substitute for smoking cigarettes or cigars. According to the National Institutes of Health, chewing on an average-sized piece of chewing tobacco for 30 minutes can deliver as much nicotine as smoking three cigarettes.
Evidence suggests that smokeless tobacco increases the risk of oral cancer, gingivitis, and tooth loss. The risk of cancer in people who use smokeless tobacco is lower than that of smokers, but is still higher than that of people who do not use tobacco at all. Using smokeless tobacco also seems to increase the risk of fatal heart attacks and strokes.
Pipes and Cigars

Pipe and cigar smoking are on the rise. Because pipe and cigar smokers often don’t inhale, the common misperception is that they don’t face as substantial a health risk as cigarette smokers. Yet recent research finds that smoking pipes or cigars causes harmful health effects similar to those of cigarettes. People who smoke pipes or cigars are at greater risk for lung damage and COPD, even if they never smoked cigarettes.
Secondhand Smoke
Secondhand smoke is produced by a burning cigarette or other tobacco product. About 88 million nonsmokers are exposed to secondhand smoke each year — 32 million of them are children and adolescents. Parental smoking has been shown to affect the lungs of infants as early as the first 2 – 10 weeks of life, and such abnormal lung function could persist throughout life.
Being exposed to secondhand smoke increases the risk for heart attacks and lung cancer. Parental smoking is believed to increase the risk for lower respiratory tract infections (such as bronchitis or pneumonia) by 50%. Exposure to secondhand smoke in the home increases the risk for asthma and asthma-related emergency room visits in children who have existing asthma. Children whose parents smoke are also more likely to be overweight and to have behavioral problems.
Quitting Smoking
It’s never too late to quit smoking. According to the American Cancer Society, about half of all smokers who keep smoking will die from a smoking-related disease. Quitting has immediate health benefits:
- 20 minutes (after the last cigarette): Blood pressure and pulse rates return to normal.
- 8 hours: Levels of carbon monoxide and oxygen in the blood return to normal.
- 24 hours: Chance of a heart attack begins to decrease.
- 48 hours: Nerve endings start to regrow. Your ability to taste and smell increases.
- 72 hours: Bronchial tubes relax and the lungs can fill with more air.
- 3 months: Improved circulation; lung function increases by up to 30%.
- 1 to 9 months: Decreased rates of coughing, sinus infection, fatigue, and shortness of breath; regrowth of cilia in the airways, improving the ability to clear mucus and clean the lungs and reducing the chance of infection; increased energy level.
- 1 year: the risk of dying from a heart attack or stroke is reduced by up to 50%.
According to the National Institutes of Health, about 40% of smokers who want to quit make a serious attempt to do so each year, but fewer than 5% actually succeed. Available smoking cessation products and therapies are greatly underused. If more smokers asked for or were offered such help, the agency says quit rates could double or triple. Methods of quitting smoking include counseling and support groups, nicotine patches, gums, lozenges, and sprays, smoking cessation pills, and slowly cutting back on the number of cigarettes smoked (incremental reduction).
Nicotine Replacement Therapy

Nicotine replacement therapy involves the use of products that provide low doses of nicotine, without the contaminants found in smoke. The goal of therapy is to relieve cravings for nicotine and ease the symptoms of withdrawal. In general, nicotine replacement therapy benefits moderate-to-heavy smokers the most. However, it does appear somewhat helpful for light smokers (people who smoke fewer than 15 cigarettes a day).
Combining nicotine replacement therapies may be more effective than using one alone. For example, a combination of the nicotine patch and nicotine gum, nasal spray, or lozenge helps smokers go smoke-free for a longer period of time before relapsing. Adding bupropion to nicotine replacement therapy also increases the chance for success.
Nicotine Patches:

Nicotine patches deliver nicotine through the skin. This is called transdermal nicotine delivery. It is effective in reducing symptoms during withdrawal. Nicotine patches are available over the counter. Patches may work in different ways:
- Step-Down Approach. Patches that use this method include NicoDerm CQ. The patches come in three strengths (21, 14, and 7 mg). You use the strongest dose first and reduce it gradually over a period of 8 – 10 weeks. A 21 mg patch is about equal to 15 cigarettes. A heavy smoker may need to wear two patches at first.
- Single-Step Approach. The single-step patch (Nicotrol) can be taken off after 16 hours and replaced 8 hours later. It can be used for only 6 weeks.
Patches are applied and used in similar ways:
- A single patch is worn each day and replaced after 24 hours.
- To avoid skin irritation it is applied to different hairless locations above the waist and below the neck each day.
- People can wear the patches for 24 hours, but some have reported odd dreams and have disliked the sensation of the patch during the night. People who wear the patch all the time, however, have fewer withdrawal symptoms and slightly better abstinence rates than those who take it off at night.
- Patches should be stored and discarded safely, particularly in homes with small children. Small children have been poisoned and gotten sick from wearing, chewing, or sucking on nicotine patches. There have been no reports of death in children who have been poisoned.
- The FDA recommends using the patches for 3 – 5 months, although some studies suggest that using them for 8 weeks achieves the maximum benefits.
Children should not come in contact with the patches, even while the smoker is wearing them. If a child puts on a patch, it should be removed and the affected skin should be washed right away. Urgent medical care may be required if the child has eaten nicotine or worn a patch for a prolonged time.
Nicotine Gum:


Nicotine gum (Nicorette) is available over the counter and has helped many people quit. Some people prefer gum to the patch because they can control the nicotine dosage, and chewing satisfies the oral urge associated with smoking. Tips for using the gum:
- If you are just starting to quit, chew 1 – 2 pieces every hour or two. Do not chew more than 24 pieces a day.
- Gradually taper off. The goal is to stop using the gum by 3 months, but about 3% of people continue to use it long after they have quit smoking.
- Chew the gum slowly until it develops a peppery taste. Then tuck it between the gum and cheek, so that the nicotine can be absorbed.
- Coffee, tea, soft drinks, and acidic beverages may interfere with nicotine absorption, so wait at least 15 minutes after drinking before chewing a piece of gum.
The Nicotine Inhaler: The nicotine inhaler resembles a plastic cigarette holder. It comes with a number of nicotine cartridges, which are inserted into the inhaler and “puffed” for about 20 minutes, up to 16 times a day. The dose is gradually decreased. It requires a prescription in the United States. Several studies have reported that the inhaler triples abstinence rates (between 17 – 28%) compared with placebo (6 – 9%) after 6 months. It has some specific advantages over other nicotine replacement products:
- The inhaler provides varying doses of nicotine on demand (as opposed to continuous doses with the patch or gum) and is relatively fast-acting. Blood nicotine levels peak about 20 minutes after using the inhaler, comparable to the gum and faster than the 2 – 4 hours seen with the patch.
- It satisfies oral urges.
- Most of the nicotine vapor is delivered in the mouth, not into the lung airways (although some people experience mouth or throat irritation and a cough).
- Using a combination of the inhaler and the patch may be particularly effective.
Electronic cigarettes (E-Cigarettes):

Electronic cigarettes are cigarette-, cigar-, or pipe-shaped devices that deliver nicotine or other substances in the form of a vapor. Electronic cigarettes are marketed as quit-smoking aids because they are designed to give the feeling of smoking without actually lighting up. However, the FDA cautions that electronic cigarettes have not been carefully evaluated for safety or effectiveness. In 2010, the FDA issued warning letters to five distributors of electronic cigarettes for violations including unsubstantiated claims and poor manufacturing processes. The agency wants manufacturers to conduct clinical studies to determine whether their products are actually safe and effective.
Nicotine Lozenge: A nicotine lozenge (Commit) is available over the counter. It is made from pressed tobacco and comes in two strengths for heavier or lighter smokers. Suck on one piece every 1 – 2 hours, then gradually taper off your use. Don’t eat or drink 15 minutes before using a lozenge, and don’t take more than 20 lozenges a day. Side effects include heartburn, hiccups, nausea, headaches, and cough. The Commit lozenge also contains phenylalanine, a chemical that certain people may need to avoid.
Facts about Nicotine Replacement Therapy
- Not cheating on the very first day of nicotine-replacement use increases the chance of quitting permanently tenfold.
- The more cigarettes people smoke, the higher the dose of nicotine replacement they may need at first.
- Adding a counseling program may boost the effectiveness of any nicotine replacement program.
- Do not smoke while using nicotine replacement. It can cause nicotine to build up to toxic levels in your body.
- Nicotine replacement helps prevent weight gain while you are using it, but you are still at higher risk for gaining weight when you stop using all nicotine.
Side Effects: Side effects of any nicotine replacement product may include headaches, nausea, and other gastrointestinal problems. People often experience sleeplessness in the first few days, particularly with the patch, but the insomnia usually passes. Patients using very high doses are more likely to have symptoms. Reducing the dose can prevent these symptoms.
Special Concerns for Specific Individuals: There has been some concern that the patch might be harmful for people with heart or circulatory disease, but studies are finding that it poses no danger for these individuals. In fact, the patch may help reduce angina attacks brought on by exercise. However, unhealthy cholesterol levels (lower HDL levels) caused by smoking remain abnormal with use of the nicotine patch. HDL levels improve when all nicotine is stopped.
Smoking Cessation Pills
Bupropion (Zyban) is a type of antidepressant that is also an FDA-approved product for smoking cessation. It differs from most other antidepressants because it increases the effects of dopamine, the brain chemical that appears to play a strong role in nicotine addiction. Using bupropion along with nicotine replacement therapy may help you better control cigarette smoking cravings. Bupropion does not contain nicotine. In most cases, bupropion is started a week or two before quitting, and must be taken for 7 – 12 weeks. The usual maintenance dose is a 150 mg tablet twice a day. No single dose should be higher than 150 mg.
Side effects of bupropion include gastrointestinal problems, headaches, insomnia, dry mouth, and irritation. In very rare cases, seizures have occurred, although usually in people who exceeded the recommended dose or who already had risk factors for seizures.
Warning about Bupropion: In July 2009 the FDA required the makers of bupropion to add a Boxed Warning (the strongest possible warning) regarding serious mental health side effects that may occur while using the medication. These potentially serious side effects include “changes in behavior, hostility, agitation, depressed mood, suicidal thoughts and behavior, and attempted suicide.” Patients taking this medication, as well as their family members, should be aware of these potential dangers and report any symptoms to their doctor immediately. Patients are also advised to stop taking the medication immediately if any of these symptoms occur.
Nortriptyline (Pamelor, Aventyl) may help reduce nicotine action. Quit rates with this medication are as high as 30%. Long-term abstinence rates are more than twice those of placebo. Most other antidepressants, including fluoxetine (Prozac), have no additional benefits for smokers. Nortriptyline has been specifically studied for helping smokers. It is best to start taking the medication 10 – 28 days before your intended quit date. Side effects of nortriptyline include drowsiness, dry mouth, and changes in taste. In rare cases, tricyclic antidepressants can have serious side effects, and an overdose can be deadly. Tricyclics may pose a danger for patients with certain types of heart disease.
A newer drug called Varenicline (Chantix) may significantly work better than bupropion. Unlike bupropion, it works on nicotine receptors in the brain, which helps reduce cravings. Varenicline can be used by cigarette smokers ages 18 and older. It should not be combined with nicotine replacement therapy. Nausea is one of the side effects. Warning about Chantix: Varenicline carries a Boxed Warning regarding serious mental health side effects that may occur while using the medication, or immediately after stopping it. These uncommon but potentially serious side effects include “changes in behavior, agitation, depressed mood, suicidal ideation and suicidal behavior.” Patients taking this medication, as well as their family members, should be aware of these potential dangers and report any symptoms to their doctor immediately. Patients are also advised to stop taking the medication immediately if any of these symptoms occur.
Behavioral Methods and Counseling

Everyone who quits should aim to quit completely. Most people who return to smoking “cheat” in the first few weeks. Quitting completely is essential to regaining good health and reversing the harmful effects caused by smoking. Reducing smoking, even by half, does not eliminate the risk for cancer and other health problems. Although smokers who cut back take in less smoke and nicotine, their bodies are still unable to heal completely from the ongoing intake of toxins. Changing to low-tar cigarettes is not a solution. In fact, people who smoke these cigarettes tend to inhale more deeply, perhaps even increasing their health risks.
Create a List: Write down 10 reasons to quit. In addition to health reasons, the list might include having better smelling hair, clothes, and breath; having fewer wrinkles; enjoying the taste of food; and saving money. Read the list often during the quitting process to help you stay motivated. If quitting cold turkey isn’t for you, gradually stopping is an equally effective approach, according to research. Reducing the number of cigarettes you smoke before quit day might work just as well as stopping all at once.
Decide on a Specific Quit Date: Some people find it helpful to choose a particular date to quit when they anticipate little or no stress for at least the first 3 days. Women affected by PMS should avoid quitting right before getting their period. It may help to write out a quit contract, putting the date on paper, and get a friend to sign it. Discard all smoking paraphernalia on the eve before the quit date, and make plans to stay busy on the day itself, especially at night, when the urge to smoke will be high.
Make an Oath
Take an extreme oath. For example, “If I smoke one more cigarette my dog will die.” Although this seems absurd, some people, even well-educated individuals, who have failed all other methods have reported that they quit completely and successfully after taking such an oath. Let the Body and Mind Heal During Withdrawal:
- Retreat from the world when cravings become overwhelming. Take naps, warm baths or showers, meditate, or read novels.
- Help your body get rid of nicotine. Drink plenty of water; eat fresh fruits, vegetables, whole grains, and fiber-rich foods. Carrots, apples, and celery are good munching foods.
- When cravings occur, hold your breath for as long as possible, or take a few deep rhythmic breaths.
- Use meditation or relaxation and deep breathing exercises. In fact, taking deep breaths when the urge to smoke occurs is a good stopgap measure.
Get Family and Friends Involved

- Tell all your friends and family that you’ve already quit, so you’ll be embarrassed if they catch you smoking.
- Fine yourself. Pay a family member or friend if they catch you smoking. The amount should be large enough ($5 – $20) to be a deterrent, but not so large as to be ridiculous. Even better — donate the money to charity.
- If your partner or friend smokes, try persuading them to quit or, at the very least, not to smoke around you.
Change Daily Habits
- Change your daily schedule, particularly eating times, as much as possible. Eat at different times or eat many small meals instead of three large ones. Sit in a different chair or even a different room.
- If you smoke after eating, find other ways to end a meal. Play a tape or CD, eat a piece of fruit, get up and make a phone call, or take a walk (a good distraction that burns calories as well). For example, if you normally have a cigarette with coffee, drink tea instead or use a different cup.
- Substitute oral habits by eating celery, chewing sugarless gum, or sucking on a cinnamon stick.
- Go to public places and restaurants where smoking is prohibited or restricted.
- Set short-term quitting goals and reward yourself when you meet them.
- Every day put the money you’d normally spend on cigarettes in a jar and buy something pleasurable at the end of a predetermined period of time.
- Find activities that focus the hands and mind but are not taxing or fattening, such as playing computer games or solitaire, knitting, sewing, or doing crossword puzzles.
About 4% of smokers who quit without any outside help succeed. Nevertheless, most people try to quit alone, and many have reported that certain activities can help the process of withdrawal. The primary obstacle in trying to quit alone is making the behavioral changes needed to eliminate the habits associated with smoking. Excellent books, CDs, and manuals are available and are strongly recommended to help people who want to quit without other assistance.
Smokers who use outside help have the best record for quitting, with success rates of 25% – 35%. Those who are counseled in addition to using nicotine replacement and Zyban have the best chance of quitting. Varenicline can double or triple your odds of quitting. Brochures, CDs, and other self-help materials are often ineffective when used alone, but they may be helpful in conjunction with a counseling program.
Alternative Methods for Quitting
Hypnosis: Although rigorous studies are lacking, some people report successful smoking cessation when they receive hypnosis in individual sessions. Hypnosis is effective only if you trust the therapist and can feel completely at ease in the vulnerable and passive state necessary for hypnotic suggestion. During a typical session, the hypnotherapist will use various techniques (such as imagery and silent counting) to put you in a relaxed state.
When you are very relaxed, but not asleep, the hypnotherapist will quietly suggest motivations for not smoking. The hypnotherapist should also reinforce a positive self-image while you are in deep relaxation. This helps many people avoid the depression that accompanies withdrawal. The sessions usually take about 1 hour. You should be taught methods of self-hypnosis to use at home, and follow-up once to reinforce what you’ve learned.
Acupuncture and Acupressure: There is no real evidence that acupuncture helps people quit smoking, although this method is safe to try. The acupuncture technique for quitting smoking usually uses very tiny curved staples inserted into three different points around the edge of the ear. The procedure is painless. You will be told to press each staple in a certain order for a few seconds whenever you crave a cigarette. The acupuncturist may also use acupuncture points elsewhere on the body. There are no side effects, except for some soreness if the acupuncture staple is pressed too hard.
A related technique called acupressure involves simply pressing select points on the body when a craving hits. Some studies have reported good quit rates with acupuncture, but few rigorous studies have been conducted using acupressure.
Symptoms of Withdrawal

After you quit smoking, you will have some withdrawal symptoms. Such symptoms generally peak in intensity 3 -5 days after you quit, and usually disappear after 2 weeks, although some may persist for several months. The symptoms of withdrawal are both physical and mental.
Physical Symptoms: Tingling in the hands and feet sweating, intestinal disorders (cramps, nausea), headaches, sore throat, coughing, and signs of a cold. Withdrawal symptoms should be treated just like physical symptoms due to an illness or disease.
Mental and Emotional Symptoms: Tension and cravings build up during periods of withdrawal, sometimes to a nearly intolerable point. Nearly every moderate-to-heavy smoker experiences more than one of the following strong emotional and mental responses to withdrawal:
- Temper tantrums, intense needs, feelings of dependency, and a state of near paralysis.
- Insomnia, mental confusion, vagueness, or difficulty concentrating.
- Irritability, restlessness, impatience, or anger. Anxiety and depression.
- The first signs of nicotine withdrawal can appear within 30 minutes of a smoker’s last cigarette. Within 3 hours, the person may experience anxiety, sadness, and difficulty concentrating.
Regular Check-Ups

If you smoke, you should be screened for any smoking-related disorders. Have your cholesterol and blood pressure checked regularly. Women should have regular Pap smears to detect cervical cancer (the required frequency of the Pap smear varies by age and medical history, such as exposure to the human papillomavirus). All older adults should be screened for colon cancer.
A note about computed tomography: Computed tomography (CT) screening programs are becoming increasingly available. These programs may claim that they can successfully detect lung cancer early. However, to date, these programs are experimental at best, and in controlled studies they offer no survival benefits for lung cancer patients.
